The paramedic placed pads and defibrillated within one minute. Shortly after transport commenced, the patient became unresponsive with Torsades de Pointes, which rapidly degenerated into ventricular fibrillation. He had a previously undiagnosed atrial fibrillation with rapid ventricular response and left bundle branch block, but was alert. A 61-year-old male presented with a one-week history of chest pain and shortness of breath. Read more about Wide QRS Complex With First-degree AV BlockĪ paramedic crew responded to the office of a local physician.There is left axis deviation in the frontal plane and poor R wave progression in the horizontal plane. 12 seconds, or 120 ms., representing interventricular conduction delay (IVCD). The ECG: The rhythm is sinus at around 60 bpm, although the rate varies a little at the beginning of the strip. He was started on chemotherapy for multiple myeloma and will be followed as an outpatient. There was suspicion of renal and cardiac amyloidosis, but the patient refused biopsy to confirm this. He presented with a complaint of nausea and vomiting and was found to have a worsening of acute kidney infection. He has a recent diagnosis of IgA myeloma. He also suffered deep vein thrombosis and is on anticoagulation. The Patient: This ECG was taken from a 73-year-old man with a history of heart failure with preserved ejection fraction, severe left ventricular hypertrophy, Type II diabetes, and stage 4 chronic kidney disease. The ST depression in the inferior wall is most likely reciprocal. After the offending artery was opened and stented, the wide complex became narrow and was considered to be an interventricular conduction delay that was due to the ischemia. However, it doesn’t have the “look” of LBBB with the low-voltage seen in the anterior wall. The wide QRS meets the criteria for left bundle branch block (wide QRS, negative QRS in V1 and positive QRS in V6 and Lead I). This was confirmed in the cath lab, as the patient had an occlusion of the left anterior descending artery near the bifurcation of the circumflex. 
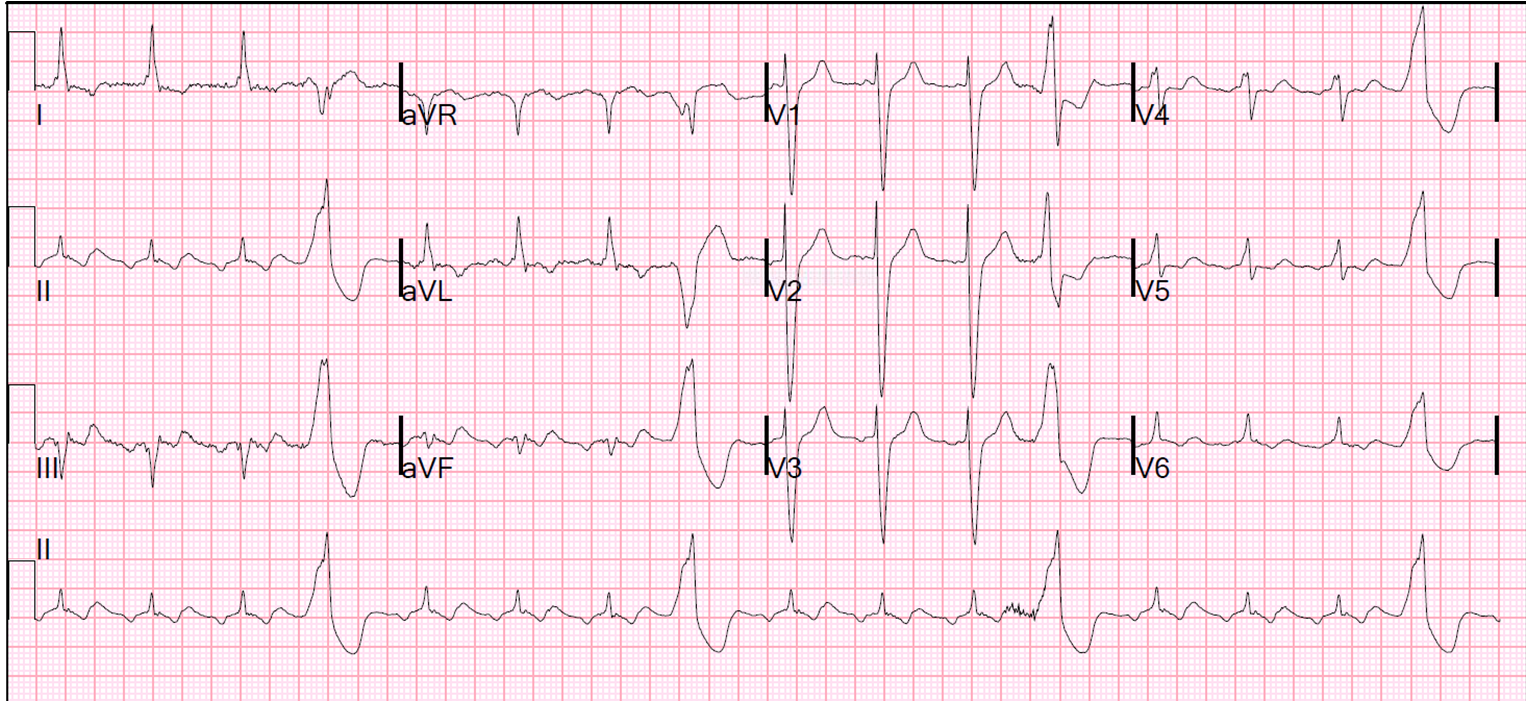
is extensive, covering the entire anterior wall, and extending into the high and low lateral walls. Interpretation: The rather obvious ST-elevation M.I. With his symptoms and this alarming ECG, he was sent promptly to the cath lab. Lead II is equally biphasic while I and aVL are positive, indicating an axis that is shifted slightly to the left. There is ST depression in the inferior leads, II, III, and aVF. There is also ST elevation in aVL with ST straightening in Lead I. The shape of the ST segments in the anterior wall range from coved upward in a “frowning” shape (V1) to very straight (V5 and V6). There is ST segment elevation in all precordial leads, except for possibly V6. The ECG: The rhythm is normal sinus at a rate of about 76 bpm with normal intervals. The Patient: An elderly man presents with chest pain, pallor, diaphoresis and weakness. Read more about Non-specific IVCD With Peaked T Waves.There are no pathological Q waves, unless we count V1, which may have lost it’s Q wave as part of the general poor R wave progression. The ST segments are generally concave up, and the J points are at the baseline – no ST elevation or depression. V1 through V4 look almost the same, small r and large S. This is very close to being wide enough for a diagnosis of left bundle branch block, and represents poor conduction throughout the ventricles. On the chest leads side, there is poor R wave progression. AVR is equiphasic – the axis travels perpendicular to the positive electrode of aVR, toward the patient’s left shoulder. Notice that Leads II, III, and aVF are all negative. The frontal plane QRS axis is -56 degrees – abnormally leftward. The PR interval is 155 ms (.15 seconds), and the P waves are upright in the inferior leads. The ECG: The rhythm is sinus at 97 bpm (fast for this patient). We do not have other history available to us. He had a history of CHF and hypertension. The Patient: This ECG was obtained from an elderly man who was suffering an exacerbation of congestive heart failure.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
